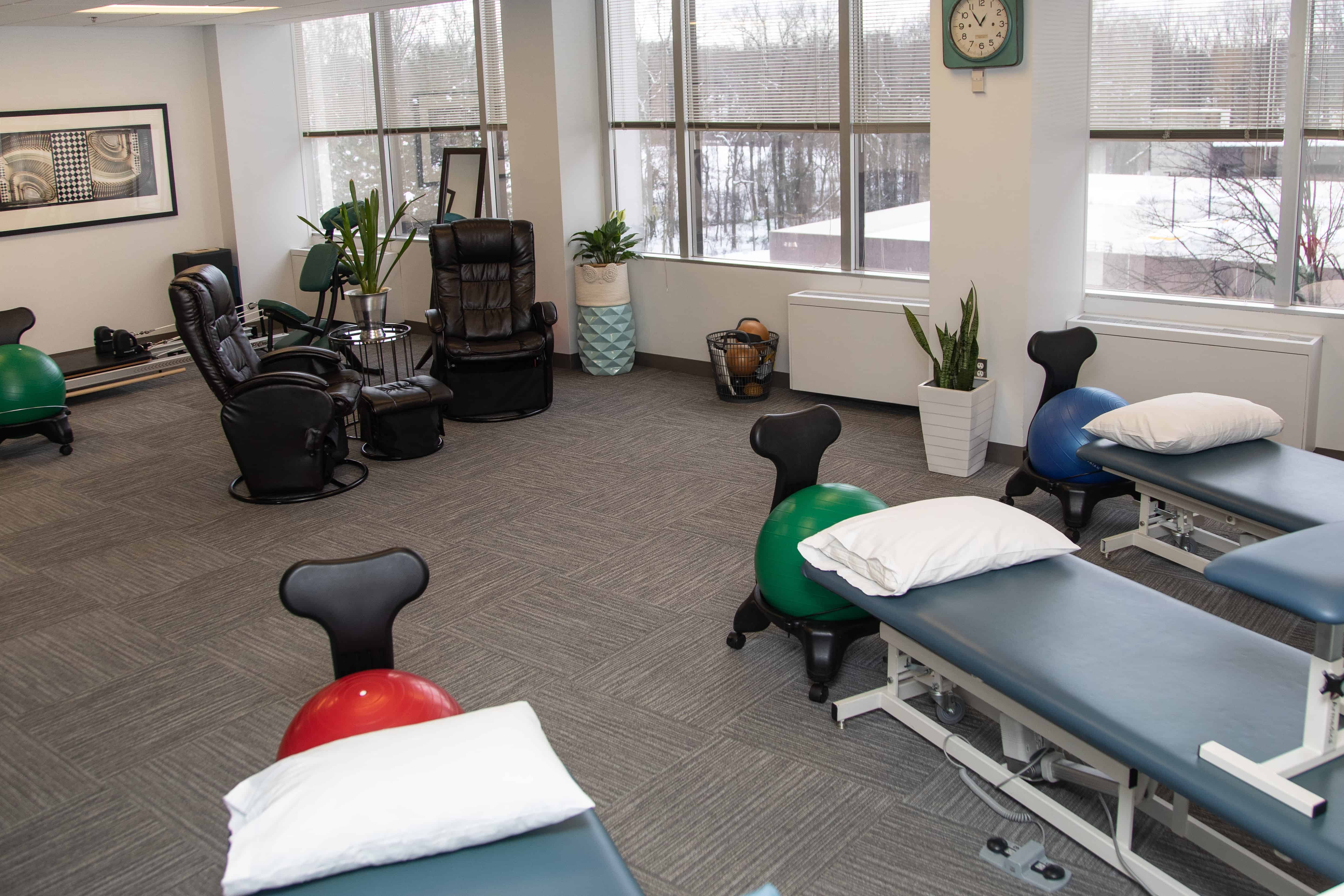
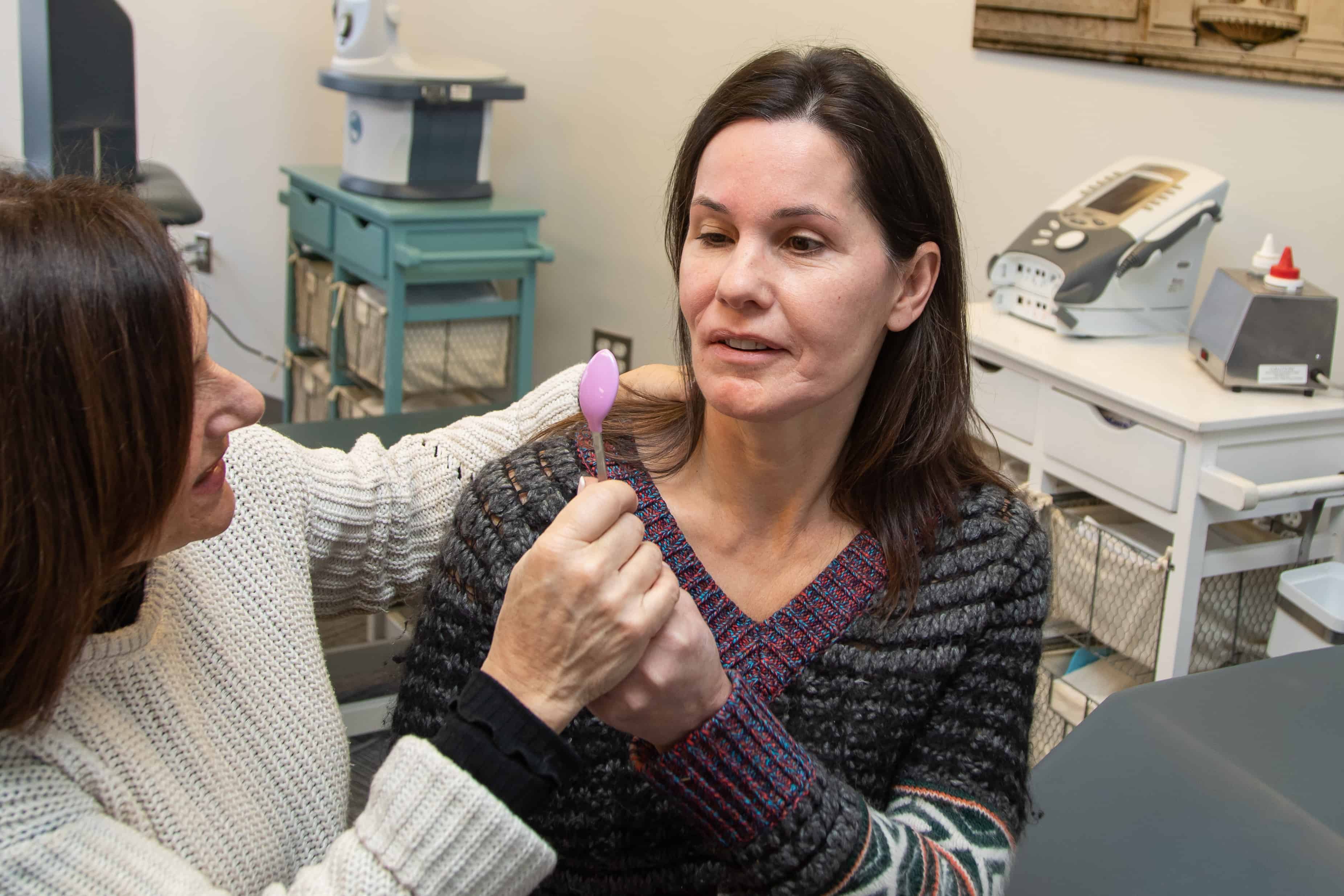
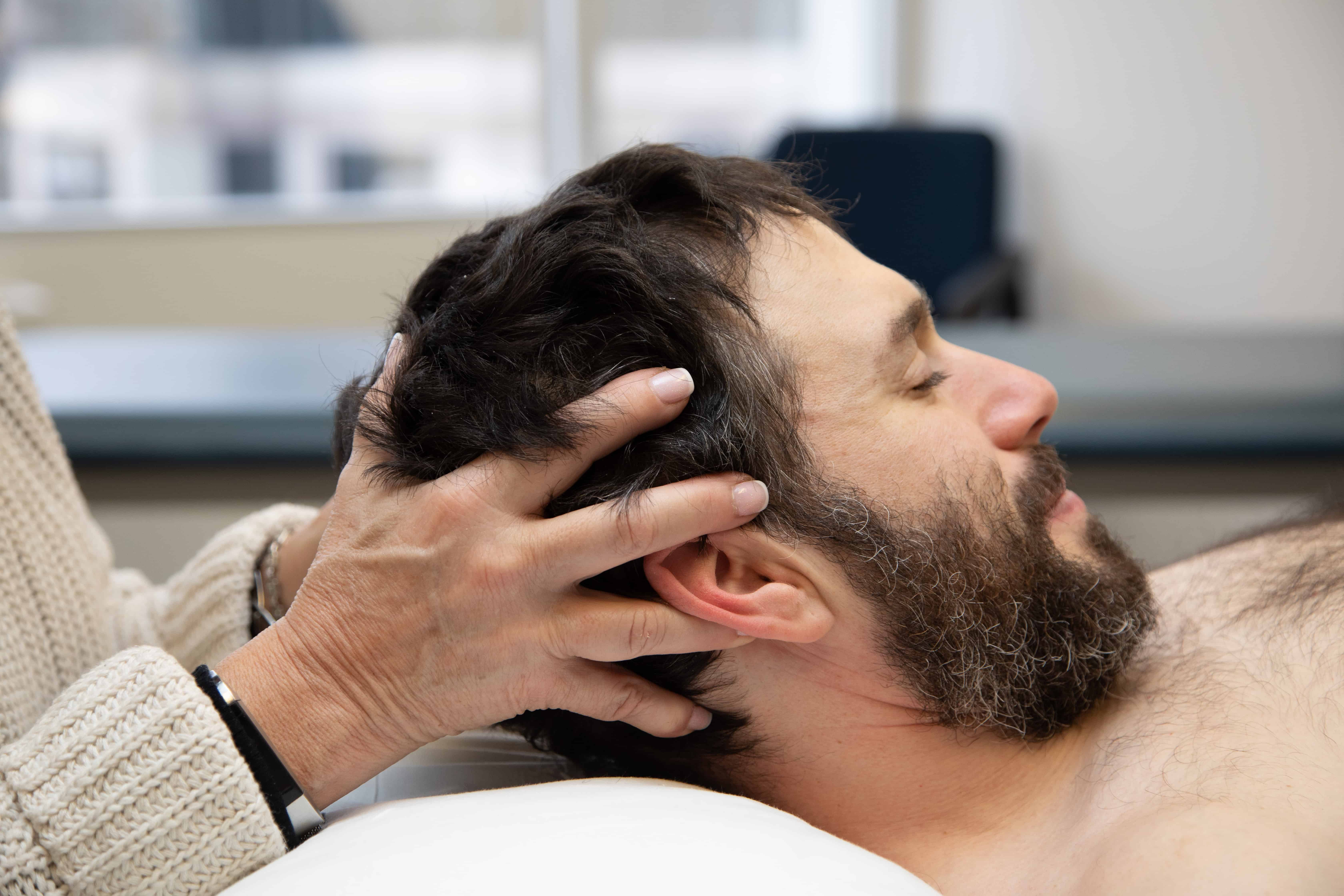
Our practice is about making a difference through knowledge, compassion, and dedication. For many years, we have treated patients who have been on a very long road with many detours to find the care they needed and deserved. It was our passion to open a center that was dedicated to the treatment of patients with facial weakness/abnormal movement, TMD, posture/neuromuscular imbalances, and pelvic floor dysfunction. Our promise to you is that we will be 100% committed to your recovery and provide you with the education and skills you need to understand and manage your diagnoses. At CFFR, you are the center of your recovery. We will educate you regarding your condition, treat your symptoms, listen to your concerns, and look beyond your diagnosis to treat the whole person. Our head-to-toe approach of analyzing your condition allows us to use our skilled, hands-on techniques to provide you with the highest quality of physical therapy care. Working with patients on their paths to recovery is our passion. We are clinicians who learn more and more every day from our patients allowing us to provide you with very unique and dynamic interventions.
You have facial palsy or TMD and are told you will either get better or not. You are given no guidance, so you head to the internet where you can find a lot of false and misleading information. You are frustrated because you just were stricken and you have a lot of questions and are getting no answers. Or maybe it has been three months and you are not fully recovered and are trying to discover if there is anything you can do to improve your recovery. Or you have had symptoms for several years or decades and are wondering if there are any new treatments. So many of our patients come to us having wandered through a complex, confusing, and splintered health care system, getting mixed messages about the best treatments. We help you navigate the process and provide you with an individualized treatment plan that is coordinated with your entire medical team.
Facial Palsy
Facial palsy occurs when there is a decrease in or failure of communication between the facial nerve (cranial nerve VII) and the facial muscles. This results in loss of the facial movement that controls expressions. In other words, it causes the nerves, typically on one side of the face, to stop working, making it difficult to close one eye, smile, or even drink from a cup or straw. It can be very debilitating mentally and physically.
The cause of Bell’s palsy (BP) is still being debated in the medical literature. Many times, this term is used generically to describe facial palsy. Two theories include causation from the herpes simplex virus or an inflammatory process that is not viral in nature.
Ramsay Hunt Syndrome (RHS) is caused by the herpes zoster virus and is described as “shingles to the facial nerve.” Eruption or multiple eruptions are noted in or around the ear and mouth regions. Multiple cranial nerves can be impacted with symptoms such as sensitivity to sound and/or light; balance disturbances (dizziness); pain that lingers after the facial weakness develops; changes in sense of taste; and increased headaches.
Zoster sine herpete (ZSH) is also caused by the zoster virus, but does not produce a rash (eruptions). However, all of the other symptoms outlined above can occur.
Additional causes include:
- Damage to the nerve as a result of surgery, such as removal of an acoustic neuroma or a parotid tumor
- Cancerous tumors of the face, head, or neck region
- Bacterial causes such as Lyme Disease or following a middle ear infection
- Neurological conditions such as Neurofibromatosis 2 or Guillain-Barré syndrome
- Traumatic injury to the facial nerve
- Birth trauma
- Congenital conditions
Learn more at The National Institutes of Health.
The main signs of facial palsy typically include, but are not limited to, facial weakness or unilateral paralysis, dry mouth and/or eye, and problems tasting. These symptoms can occur suddenly, in as quickly as 24-48 hours. Many people experience severe pain behind their ear or in the back of their head several hours prior to the onset of facial weakness. Because these symptoms are the same as in other serious conditions, it is imperative that you see your physician immediately upon experiencing any of the above symptoms.
At CFFR, we specialize in the treatment of all phases of facial palsy from those in early onset to longstanding patients who have developed synkinesis. The advantages to early intervention include implementing patient eye-care education, understanding the disease process, initiating home exercises, and, if necessary, connecting you to a physician who is experienced in the treatment protocols for your diagnosis. Our individualized treatment programs include a comprehensive approach utilizing neuromuscular re-education; manual therapy techniques; diagnostic ultrasound; graded motor imagery; biofeedback; SynkineedingTM; IBBS; and modalities, such as laser therapy, vasopneumatic devices, therapeutic ultrasound, and radial pulse therapy.
You should be evaluated by a physician! If you don’t have one, we will gladly provide you with the contact information for a physician with expertise in treating facial palsy. According to May and Schaitkin, doctors and authors of The Facial Nerve, there have been 113 different causes for facial weakness identified in related literature. It is essential to receive a quick and accurate diagnosis. This will allow your medical provider (neurologist, ENT, primary care, or ER doctor) to initiate the correct plan of care. On your first visit, we will review your medical plan of care to confirm that current practices in the management of facial paralysis have been utilized.
Based on the cause, the course of recovery varies significantly and ranges from weeks to years. It is imperative to have an accurate diagnosis at onset because the course of treatment will vary. Diagnostic tools include an MRI of the facial nerve, CT scan, bloodwork, hearing test, vestibular assessment, vision screening, and a thorough physical exam.
Bell’s Palsy Association
Sir Charles Bell Society
Acoustic Neuroma Association
Bell’s Palsy Fact Sheet
For more information on neurological disorders or research programs funded by the National Institute of Neurological Disorders and Stroke, contact the Institute’s Brain Resources and Information Network (BRAIN) at:
BRAIN
P.O. Box 5801
Bethesda, MD 20824
www.ninds.nih.gov
TMD
Disorders of the temporomandibular joint (TMJ) have been reported as far back as the ancient Egyptians. Problems with the jaw are known as temporomandibular joint disorder or dysfunction (TMD). TMD is very common; in fact, according to the U.S. Department of Health and Human Services, there are more than ten million Americans affected by this disorder. TMD symptoms include jaw pain; jaw fatigue; difficulty opening the mouth to eat, talk, or yawn; ringing in the ears; dizziness; headache; popping or clicking sounds in the jaw; facial pain; tooth pain; pain behind the eyes; neck pain; and shoulder pain/weakness.
Poor postural habits. One of the reasons TMD is so common is because many people spend a great deal of time sitting at a desk with poor posture where the head is too far forward and the spine is rounded. This puts a strain on the muscles, discs, and ligaments of the TMJ, neck, back, and shoulders. Utilizing electronic devices such as cell phones, tablets, and computers for prolonged periods of time is another chief cause of poor postural habits.
Stress. Stress often causes chronic jaw clenching (bruxism) which can lead to muscle tension/spasm.
Malocclusion. Problems with one’s teeth not aligning properly may cause increased stress on your TMJ and surrounding muscles.
Fracture. In a traumatic accident involving the face or head, a fracture to the lower jaw may result. Even after the fracture has fully healed, TMJ stiffness and pain may remain.
Surgery. Following surgery to the face, jaw, neck, or shoulder, there may be a loss in mobility and function of the TMJ and surrounding anatomy.
Trismus (lockjaw). This condition – where jaw muscles spasm and the jaw cannot be fully opened – can be both a cause and a symptom of TMD. Other causes of trismus include trauma to the jaw, tetanus, and radiation therapy to the face and neck.
Whiplash injuries. TMD may be caused by injuries involving a severe jerk of the head; these often occur due to falls, sports-related mishaps, or automobile accidents.
Concussion. A concussion causes trauma inside the skull. It can also injure the junction between the skull and neck – which can have a significant impact on the TMJ region.
Learn more at The Washington Post.
Postural evaluation is a key component to our assessment and treatment of TMD. What makes our approach different is that we understand that the body is a chain and that a kink anywhere along the chain must be addressed in order to achieve lasting relief from dysfunction. We start at your feet and work all the way up to your jaw. When necessary, we work very closely with our team of dental and musculoskeletal specialists and podiatrists to allow for biomechanical alignment and symptom management.
Manual therapy techniques are utilized to improve joint mobility and decrease muscle spasm in the jaw, spine, and extremities for successful pain relief.
Neuromuscular retraining represents a series of therapy techniques which will help restore normal function of nerves and muscles. Muscles have memory and patients who have experienced muscle pain often have “bad muscle memory.” Our program retrains muscles and the brain to remember what it is like to move an area correctly without pain.
Modalities are various interventions used to help decrease pain and dysfunctional movement. Sometimes called “therapeutic modalities” or “physical modalities,” these are used in conjunction with your PT program to help you feel better and increase mobility, as well as strengthen, relax, and heal muscles. The specific modalities that we choose for each patient vary depending on conditions, needs, and rehab goals. At our Center, modalities include dry needling, ultrasound, electrical stimulation, laser, vasopneumatic, and radial pulse therapies.
Additional Questions
We highly recommend that all initial visits be conducted at our office. We provide flexible treatment times and days to meet your schedule. That said, we are proud that our practice treats patients all over the world using HIPAA-compliant telehealth technology. We can provide our patients with home therapeutic devices and guide them in using this equipment, as well as offer links to mobile apps to enhance their recoveries.
The cost of treatment is tied directly to each patient’s individualized treatment plan. The center has chosen to practice independently of managed healthcare networks. This allows us to spend the appropriate amount of time to fully examine, discuss all aspects of your disorder, and maintain a high quality of care. We do, however, believe in holding down costs in order to increase access to the level of care that our patients need and deserve.
It depends on your personal insurance plan, so you should always check with your health plan carrier. We have provided a document to assist you with determining your insurance benefits for physical therapy. Most plans do cover treatment, typically up to 80%. At CFFR, our patients pay for treatment directly and our administrative support team will provide you with the necessary documentation to submit your claim. Please use this Insurance Worksheet to help guide you through the process.
Additionally, we are pleased to be a CareCredit provider center. CareCredit is a healthcare credit card designed for your health and wellness needs. This payment option is different from a regular credit card and may be used to pay for out-of-pocket expenses not covered by medical insurance. Special financing options are available that you may not be able to get with other cards. Learn more.
We’d be happy to answer all of your questions. Please contact us today.